Report: Gen Z Leaving Healthcare in Droves Due to Toxic Culture

What You Should Know:
– A new report from Soliant Health reveals a concerning trend: healthcare professionals across all age groups are leaving the industry due to job stress, poor work-life balance, and unhealthy workplace cultures.
– Surprisingly, Gen Z (ages 18-27) is leading the exodus, with over 22% planning to leave their healthcare jobs within the next 1-3 years.
Generational Differences in Departure Drivers
While all generations struggle with workplace challenges, the Soliant Health 2024 Healthcare Employment Trends Report identifies specific concerns for each age group:
Gen Z: Unhealthy workplace culture and limited career advancement opportunities are the primary drivers for leaving.
Millennials (ages 28-43): High job stress, burnout, and poor work-life balance are the main concerns.
Gen X (ages 44-59): Similar to Millennials, unhealthy workplace culture and high job stress are top concerns, along with lack of support from management.
Baby Boomers (ages 60+): Unhealthy workplace culture, job stress, and lack of leadership support are the main reasons for leaving.
Strategies to Improve Retention
The report offers key strategies for healthcare organizations to address these challenges and improve retention:
Promote Work-Life Balance: Offer flexible scheduling, reduce overtime, and consider telemedicine or part-time options.
Improve Workplace Culture: Foster positive and inclusive environments through feedback, employee engagement, and open communication.
Prioritize Career Advancement: Provide mentorship, leadership training, and continuing education opportunities, especially for younger generations.
Enhance Leadership Support: Strengthen relationships between staff and management through regular check-ins and collaborative problem-solving.
“The Soliant Health 2024 report confirms that addressing the diverse and evolving needs of healthcare professionals is key to retaining a dedicated workforce,” said Washburn. “Organizations must focus on holistic strategies to reducing job stress, promoting work-life balance, and fostering a healthy workplace culture if they want to keep their employees engaged and committed.”
by Fred Pennic 11/15/2024

Arizona’s future prosperity depends on wellness and positive mental health. The COVID pandemic crushed us. Stress, anxiety, low self-esteem, substance abuse, burnout, absenteeism, suicidal thoughts, and lack of job engagement damaged our community’s cohesiveness, economic health, and productivity.
And mental health challenges continue to escalate in today’s hypercompetitive environment, inflationary uncertainty, polarized politics, technological job obsolescence, supply chain risks, and pressures to upgrade workforce skills.
The Wake-up Call
Arizona ranks an appalling 49th, as measured by the high rate of mental illness and low access to care (2023 State of Mental Health in America). Our mental health system is struggling to keep up with tremendous service demand, particularly for low-income, minority, elderly, and student populations.
We Must Act Now
No single organization can address this complex challenge alone. We must collaborate decisively across healthcare, government, business, education, and non-profit organizations.
The best strategy to achieve a positive mental health and wellness culture in the workplace, schools, and communities is through collaborative action.
After extensive discussions with Tucson area leaders in the mental health field, three priorities for collaborative action emerged:
Priority No. 1: Accelerate Training
First and foremost, mental health professionals must be available to handle the exploding demand for services.
Arizona faces a severe shortage of workers in mental health occupations — presently, there are over 4,600 unfilled positions state-wide and 560 in Tucson.
It is a profession with high stress, long hours, and low pay.
Healthcare providers are having a hard time recruiting and retaining staff.
The consequence is “health deserts” in urban and rural areas, lengthy appointment waits times, and growing health injustice.
Businesses, governments, universities, community colleges, and healthcare providers need to forge innovative training partnerships.
Attracting students, and fast-tracking them through an accelerated curriculum, job internships, and certification status — can produce remarkable benefits.
An outstanding example is the Pima Joint Technical Education District (JTED), which works jointly with businesses and multiple school districts. JTED is building an Innovative Learning Campus which will house the Mel and Enid Zuckerman Center for Health and Medical Careers, offering programs in licensed nursing assistants, medical assistants, and public health.
To make mental health careers attractive, higher pay will be essential, and changes in insurance reimbursement rates for healthcare providers are needed.
Priority No. 2: Integrate Social Determinants of Health
Let us build on existing community pillars of strength to cooperate and collaborate for a comprehensive solution to the crisis.
Managing the underlying factors contributing to behavioral health disorders and inequities is crucial for developing sustainable solutions.
Let us energetically address existing crises of unemployment, poverty, inequality, and social exclusion that cause distress and impact an individual’s health and wellness.
A fragmented healthcare system with delivery siloes of mental, physical, emotional, and spiritual health will only lead to suboptimal outcomes, recidivism, and inconsistent continuity of care. A coordinated approach with other sectors is needed to address underlying social determinants of health, such as housing, transportation, nutrition, employment training, and social and spiritual support.
Priority No. 3. Leverage Digital Technology
Telehealth and mobile health applications soared during COVID.
Increased R&D investment in health is a precursor of the coming tsunami of digital devices, real-time data collection, and artificial intelligence-driven diagnostics, treatment, monitoring, and deep learning applications.
Our leading researchers and innovators are working on new healthcare models that are collaborative, preventive, personalized, participatory, immersive, on-demand, data intense, and value-driven.
Arizona State University, Northern Arizona University, and the University of Arizona are well-positioned anchors for establishing Arizona as a Health and Wellness Tech Hub for conducting applied research, designing demonstrations, commercializing intellectual property, nurturing entrepreneurial startups, and creating jobs.
We believe this is the moment for action and the transformation of the behavioral health ecosystem so that more Arizonans can live healthy, prosperous, and flourishing lives.
The Collaborative Care Model Could Help Reduce the Total Cost of Patient Care
May 10, 2024. Published in Behavioral Health Business
The collaborative care model (CoCM), which integrates physical and behavioral health services, may help reduce the total cost of patient care.
That’s according to a new report from the Bowman Family Foundation, which zeroed in on research published by University of Washington (IMPACT) and the University of Pennsylvania/Independence Blue Cross (Penn/IBC) and Kaiser Permanente.
“While each of these studies has limitations, taken together (using different patient populations, payer mixes and health plan types), they provide evidence that implementing CoCM in day-to-day primary care is associated with reductions in total health care costs (THCs), and that such reductions may occur as early as the first year and may increase over 3-4 years,” authors of the report write.
Mental health and substance use disorder services remain much more difficult to access than physical health care. Many patients often rely on primary care providers for behavioral health needs.
The report highlights that PCPs prescribe the majority of psychiatric drugs. Additionally, individuals with physical and behavioral health comorbidities have a higher total cost of care.
In a collaborative care model, primary care physicians remain the main point person responsible for the care of a patient with a mental health or substance use disorder but are supported by behavioral health professionals.
“CoCM also significantly increases the capacity of the existing mental health and substance use disorder (MHSUD) delivery system,” the report said. “One “full-time equivalent” psychiatric consultant can effectively impact MHSUD treatment for as many as 3 – 8 times more patients under CoCM than could be achieved through traditional 1:1 treatment.”
In addition to improved care, the report highlights the potential financial benefits of a CoCM. Specifically, it points to an unpublished study by Kaiser Permanente Colorado, which compared patients enrolled in the plan’s Depression Care Management program that were receiving CoCM in primary care practices to those receiving the standard of care.
The research found a 13% per-member-per-month savings in the total cost of care associated with members enrolled in the CoCM compared to the standard of care group.
The report makes several recommendations to boost CoCM in the future. For starters it encourages states not already reimbursing for CoCM to do so, and that the rates should be on par with Medicare reimbursement rates.
It also encourages commercial providers to incentivize the model by reimbursing at least 30% higher than Medicare rates. Additionally, the authors of the report suggest that for both Medicare and commercial patients, there is no cost-sharing associated with CoCM services.
President Biden’s Executive Order on Artificial Intelligence
(Scientific American Excerpts) President Joe Biden signed an executive order this week that urges new federal standards for AI safety, security, and trustworthiness and addresses many other facets of AI risk and development. The broad order, nearly 20,000 words long, uses “artificial intelligence” to refer to automated predictive, wise, or generative software that can mimic specific human abilities. The White House action came just two days before the start of an international summit on AI safety organized and hosted by the U.K., during which world leaders discussed global strategy on the rapidly advancing technology.
The new order moves the U.S. toward more comprehensive AI governance. It builds on prior Biden administration actions, such as the list of voluntary commitments multiple large tech companies agreed to in July and the Blueprint for an AI Bill of Rights released one year ago. Additionally, the policy follows two previous AI-focused executive orders: one on the federal government’s AI use and another aimed at boosting federal hiring in the AI sphere. Unlike those previous actions, however, the newly signed order goes beyond general principles and guidelines; a few key sections require specific action from tech companies and federal agencies.
For instance, the new order mandates that AI developers share safety data, training information, and reports with the U.S. government before publicly releasing future large AI models or updated versions of such models. Specifically, the requirement applies to models containing “tens of billions of parameters” trained on far-ranging data. It could risk national security, the economy, public health, or safety. This transparency rule will likely apply to the next version of OpenAI’s GPT, the prominent language model that powers its chatbot ChatGPT. The Biden administration is imposing such a requirement under the Defense Production Act, a 1950 law most closely associated with wartime—and notably used early in the COVID pandemic to boost domestic supplies of N95 respirators. This mandate for companies to share information on their AI models with the federal government is a first, though limited, step toward mandated transparency from tech companies—which many AI experts have advocated for in recent months.
The White House policy also requires the creation of federal standards and tests deployed by agencies such as the Department of Homeland Security and the Department of Energy to ensure that artificial intelligence doesn’t threaten national security. The standards in question will be partly developed by the National Institute of Standards and Technology, which released its framework for AI risk management in January. The development process will involve “red-teaming,” when benevolent hackers work with the model’s creators to preemptively parse out vulnerabilities.
Beyond these mandates, the executive order primarily creates task forces and advisory committees, prompts reporting initiatives, and directs federal agencies to issue guidelines on AI within the following year. The order covers eight realms outlined in a fact sheet: national security, individual privacy, equity, civil rights, consumer protections, labor issues, AI innovation, U.S. competitiveness, international cooperation on AI policy, and AI skill and expertise within the federal government. Within these umbrella categories are sections on assessing and promoting the ethical use of AI in education, health care, and criminal justice.
Technology fueled America’s youth mental health crisis, but it can help end it
Perspective by Valerie Strauss
September 21, 2023 at 12:31 p.m. EDT, Washington Post
Sian Leah Beilock is a cognitive scientist who is the new president of Dartmouth College, the first woman to hold that position since the school was founded in 1769. An expert in, among other things, the effect of stress on academic performance, she is starting her tenure by putting health and wellness at the center of her leadership agenda with a focus on the country’s youth mental health crisis.
Among her initiatives:
· On Sept. 28, Beilock is bringing to campus Surgeon General Vivek H. Murthy and his six living predecessors to discuss the crisis and explore possible solutions.
· She created a position for Dartmouth’s first chief health and wellness officer, who will report directly to her on matters affecting all students, faculty and staff, and will oversee the implementation and assessment of Beilock’s new mental health strategic plan. That plan includes training more faculty and staff in mental health aid and suicide prevention, expanding mental health support and investing in mentorship programs for students.
· She is revamping Dartmouth’s policies about time students take away from class to address mental health issues so that they are not penalized for stepping away.
Beilock is the author of “Choke: What the Secrets of the Brain Reveal About Getting It Right When You Have To,” as well as “How the Body Knows Its Mind,” and she regularly writes about mental health and well-being in publications and news services including The Washington Post, the New York Times, NBC News and the Associated Press.
By Sian Beilock
By the time the U.S. surgeon general declared that we were in the throes of a mental health crisis in 2021, suicide attempts had risen 51 percent for young girls compared with two years prior, and twice as many young people reported feeling depressed and anxious. While the pandemic tipped the scales, the mental wellness odds had already been slipping out of our favor for the past decade.
As many experts have rightly noted, this is also the time frame social media use and mobile device ownership skyrocketed. Today 97 percent of Americans own a mobile device, and 72 percent use at least one social media platform. Years before the pandemic drove kids’ screen time up by 52 percent, psychologist Jean Twenge wrote for the Atlantic that “iGen,” born between 1995 and 2012, was a “lonely, dislocated generation,” pointing out that time spent on smartphones had replaced time-old adolescent activities such as spending time with friends, dating and even driving.
A youth mental health crisis was already brewing. The pandemic made it worse, surgeon general says.
Twenge isn’t wrong; nor are the many other voices calling for smartphone bans in schools or legally imposed age limitations to access social media. But I worry what gets lost in the conversation is that the most groundbreaking tools emerging to improve mental health care rely on these same platforms. Technology, in fact, may offer the only viable solutions to beating the mental health crisis.
As a cognitive scientist and president of Dartmouth, I have a front-row seat to how students are adapting to an increasingly digital world — sometimes in ways that can be dangerous, but also in ways that can foster the very things technology is accused of diminishing — including engagement, connectivity, and mental well-being. Beating the mental health crisis will require meeting kids where they are — on their devices.
Part of the reason we can’t do this without technology is that we simply don’t have enough mental health professionals. Of the 2.7 million young Americans experiencing severe depression, only about 28 percent are receiving consistent treatment — and that figure is lower among young people of color. What’s more, there are only 14 practicing child and adolescent psychiatrists for every 100,000 children in the United States, so it’s no wonder so many are falling through the cracks.
In a crisis, schools are 100,000 mental health staff short
A large-enough health-care workforce is far from reach. Much farther than the distance most of us are willing to keep our smartphones. I’m not advocating we dismiss the addictive nature of technology or its impact on our well-being, but it’s not the whole story. The devices we carry around all day capture a tremendous amount of behavioral data — physical activity, sleep, social interactions, to name a few — which together can offer a pretty robust picture of how we’re thinking and feeling, and help fill care gaps in cases in which frequent face time with a practitioner isn’t realistic.
Substance abuse, which is both helping drive the mental health crisis and is drastically undertreated with nearly 90 percent of sufferers going without treatment, offers an example of the power of technology to provide clinical care in underserved areas or in cases in which stigmatization prevents people from seeking the help they need. Lisa Marsch and her team at the Dartmouth Center for Technology and Behavioral Health (CBTH) created and validated the first Food and Drug Administration-cleared digital therapeutic for the treatment of opioid addiction, which provides cognitive behavioral therapy interventions though the user’s digital device and has since helped roughly double rates of abstinence by lowering the threshold for access to treatment.
Digital therapeutic tools like those developed by Marsch are clinically effective software used to screen for, diagnose and treat mental illness, and rely on us using the same digital devices that we’ve become quick to demonize.
Instead of attempting to pry the smartphones out of our kids’ hands, we can instead deploy them to help uncover what exactly is making them so sad. At the height of the pandemic, Dartmouth researcher Andrew Campbell combined mobile phone sensing and self-reported mental health data to understand how covid-19 was impacting student behavior and mental well-being, and found that students were not only more stressed and anxious than in years prior, but also more likely to engage in activities that tend to exacerbate poor mental health such as sleeping less or spending more time on their phones, especially to read pandemic-related news.
Studies have found that college students are especially susceptible to mental health problems because they tend to cluster risky behaviors such as binge drinking, smoking, sleeping less, more screen time and eating less healthy foods. It is only through our phones that we have the power to collect the data that will help us parse out what is contributing most to declining mental health and what can help speed up treatment. This matters tremendously when medical care is in limited supply, and emergency rooms are scrambling to keep up with the surge of youths coming in for behavioral emergencies.
If this sounds invasive, it’s because it is, and I’d be remiss not to raise the ethical implications that must be brought to bear. Marsch, in fact, has pointed out that when it comes to digital therapeutics, privacy considerations are paramount, and researchers and practitioners have an obligation to ensure users know the full extent of data collection they’re consenting to. Ultimately, the more relevant data we collect to understand how our behaviors contribute to mental health, the more equipped we’ll be to get to the root of the issue.
For many, the privacy gained by letting the data do the talking is worth it. Whether we like it or not, we can’t ignore the fact that young people today are struggling to connect, making it increasingly difficult for them to ask for help when they need it most. If we want to end the mental health crisis, we need to make it easier, not harder, for them to communicate. Beyond simply compiling data, technology also has a role to play in fostering connection.
When the surgeon general issued an advisory in May that the United States is facing a loneliness epidemic, I knew exactly what he meant. As a college president, I’ve noticed disconnection most in young people’s struggle to communicate with each other when confronting difficult or controversial topics, to such an extent that many choose to censor themselves entirely rather than risk discomfort.
Loneliness poses profound public health threat, surgeon general says
Many chalk this up to technology replacing in-person interaction, and it’s true that today’s young people prefer to communicate digitally. It turns out, though, that texting can actually be a powerful tool for connecting with others, especially through difficult experiences, and has been shown to reduce emotional pain. The key to prevent texting (or any technology use) from becoming harmful is proper use. For example, instead of texting when surrounded with others — even if they’re strangers — wait until you’re alone and can focus on whom you’re texting, which can create feelings of closeness.
Social media can similarly become a tool for mental well-being and connection when used correctly. Online peer groups, for instance, have been shown to drive mental health improvements for people struggling with severe illness. By sharing personal stories and opening up about coping strategies, participants experienced greater social connectedness and feelings of belonging — which may outweigh the risks commonly associated with social media.
If we allow ourselves to focus blame entirely on texting, social media and smartphones as the problem, we miss an opportunity to be smarter users of technology. What’s more, we miss an opportunity to make sure they know that it’s okay to not be okay — and that we’re here to receive that information any way they choose to give it, and to help.
Surgeon General Vivek H. Murthy, who will visit Dartmouth this month along with the six living U.S. surgeons general to join me and our community in a discussion about how we end the mental health crisis, has raised a critical question: “How do we design technology that strengthens our relationships instead of weakening them?”
The reality is, technology won’t determine whether we can overcome the mental health crisis. The adults charged with the care of our kids’ mental well-being will, and we have a responsibility to model healthier interactions with technology, and also harness its power to help us better understand, diagnose and treat mental health issues — especially for those who would otherwise go without that help. Let’s make the choice to leverage these tools rather than condemn them.
Valerie Strauss is an education writer who authors The Answer Sheet blog. She came to The Washington Post as an assistant foreign editor for Asia in 1987 and weekend foreign desk editor after working for Reuters as national security editor and a military/foreign affairs reporter on Capitol Hill. She also previously worked at UPI and the LA Times. Twitter
2023–2026 Strategic Plan for the Substance Abuse and Mental Health Services Administration (SAMHSA)
The 2023–2026 SAMHSA Strategic Plan presents a new person-centered mission and vision, highlighting key guiding principles and presenting new priorities, goals, and objectives. SAMHSA has identified five priority areas to meet better the behavioral health needs of individuals, communities, and service providers.
1. Preventing Substance Use and Overdose
2. Enhancing Access to Suicide Prevention and Mental Health Services
3. Promoting Resilience and Emotional Health for Children, Youth and Families
4. Integrating Behavioral and Physical Health Care
5. Strengthening the Behavioral Health Workforce
SAMHSA has undergirded its plan with four core principles
1. Equity
2. Trauma-Informed Approaches
3. Recovery
4. Commitment to Data and Evidence
The Alliance evaluates the strategy and determines how the Arizona behavioral health ecosystem can best execute the goals.
Read the Strategic Plan
Biden-Harris Administration Announces New Actions to Tackle Nation’s Mental Health Crisis
Actions include $200 million to scale up 988 suicide and crisis lifeline and new resources for school-based mental health services
This Mental Health Awareness Month, we honor all those experiencing mental health challenges and celebrate the mental health professionals, families, and caregivers who support them. It is clear that our country is facing an unprecedented mental health crisis impacting people of all ages. In 2021, two in five American adults reported experiencing symptoms of anxiety and depression and forty-four percent of high school students reported struggling with persistent feelings of sadness or hopelessness, exacerbated by the COVID-19 pandemic, social media, and gun violence. The Biden-Harris Administration is firmly committed to addressing this crisis.
As part of his Unity Agenda, President Biden released a comprehensive national strategy to transform how mental health is understood, accessed, treated, and integrated in and out of health care settings. Across the federal government, thanks to the President’s American Rescue Plan (ARP) and Bipartisan Safer Communities Act (BSCA), the Administration has already invested unprecedented levels of funding to expand access to mental health services. The President’s FY24 budget goes further, proposing tens of billions more to transform behavioral health services for all Americans.
Today, which is recognized as Mental Health Day of Action, and throughout Mental Health Awareness Month, the Biden-Harris Administration is announcing additional critical actions to advance the President’s mental health strategy across its three key objectives: strengthening the mental health workforce and system capacity, connecting more Americans to care, and creating a continuum of support.
Strengthen the Mental Health Workforce and System Capacity
Addressing the mental health crisis requires that we confront the severe shortage of mental health professionals and strengthen the capacity of the behavioral health care system. As a result, the Biden-Harris Administration is taking new actions this month to:
Increase the size and diversity of the behavioral health workforce. Thanks to the Bipartisan Safer Communities Act (BSCA), the Department of Education (ED) has awarded more than $280 million in funding to bolster the pipeline of mental health professionals serving in schools and expand school-based mental health services and supports. Earlier this week, ED announced $95 million of this total was awarded in grants across 35 states to increase access to school-based mental health services and strengthen the pipeline of mental health professionals in high-needs school districts. Grantees from ED’s mental health programs project that these funds will create more than 14,000 new mental health professionals in U.S. schools – including school psychologists, counselors, social workers. This month, ED also announced new funding for a center that will provide technical assistance to grantees working to address the critical need in prekindergarten-12 schools for school-based mental health service providers. This summer, the Health Resources and Services Administration (HRSA) will announce a new Behavioral Health Workforce Education and Training (BHWET) funding opportunity for approximately $8.4 million to support 16 awards to recruit and train providers to provide behavioral support to children and adolescents.
Expand access to peer support. A peer worker is someone with lived experience with a mental health and/or substance use condition, and who works with other people with similar conditions in a wide range of non-clinical activities including advocacy, navigation and linkage to resources, sharing of experience, social support, and more. In the coming weeks, the Substance Abuse and Mental Health Services Administration (SAMHSA) will release the National Model Standards for Peer Support Certification. The new standards are designed to improve consistency across peer certifications and promote quality of the growing number of peer workers across the nation.
Enhance crisis response. To ensure those in crisis have access to services, SAMHSA announced the availability of more than $200 million for states, territories, call centers, and Tribal organizations to continue strengthening 988 operations. Through the SAMHSA supported 988 Suicide and Crisis Lifeline, the network receives approximately 100,000 calls, chats, and texts each week. Later this month, SAMHSA will also announce more than $9 million in awards in cooperative agreements for community crisis response partnerships. This funding will support mobile crisis response teams to ensure adults and youth experiencing mental health crises in high-need communities receive faster access to trained mental health professionals.
Expand proven models of care. To build capacity to meet the mental health needs of Americans, the Department of Health and Human Services (HHS) awarded 15 one-year state planning grants to help states develop the necessary capacity to compete to participate in the Certified Community Behavioral Health Center (CCBHC) Medicaid Demonstration. CCBHCs provide 24/7, comprehensive behavioral health care – including crisis care – to the most vulnerable Americans regardless of their ability to pay. Thanks to BSCA, we are working to expand these clinics and help more states enter the program.
Connect More Americans to Care
Even when services are available, barriers like cost, cultural bias, and inconvenience often prevent people from accessing the care they need. On average, it takes 11 years after the onset of mental health symptoms for someone to seek treatment. To help remove these barriers, the Biden-Harris Administration is taking new actions to:
Make it easier to find help. It is simply too hard to know where to start when you or a loved one experiences a mental health challenge. That’s why HHS launched FindSupport.Gov, a brand-new, easy-to-access, free-of-charge, and user-friendly online resource for all Americans to learn how to get support for mental health, drug, and alcohol issues.
Provide mental health services in schools. To help address student mental health needs, today, CMS released an updated Medicaid School Claiming and Administrative Guide and ED released a proposed rule that would revise processes on Medicaid billing under the Individuals with Disabilities Education Act, both of which are intended to make it easier for schools to provide health services to students with Medicaid. In addition, the Department of the Interior’s (DOI) Bureau of Indian Education (BIE) initiated a Behavioral Health and Wellness Program to provide indigenous focused, evidence-based, and trauma-informed behavioral health and wellness services and resources, including an expanded tele-behavioral health BIE specific 24/7 crisis hotline, to students and staff at all BIE-funded schools, colleges, universities, dormitories, and programs.
Support mental health of workers. Work related stress and burnout can lead to mental health challenges for America’s working families. To help address workplace mental health, earlier this month, the Department of Labor (DOL) launched a Mental Health at Work Initiative to promote key resources in support employees and employers. The Occupational Safety and Health Administration (OSHA) also rolled out the Workplace Stress Toolkit to provide guidance and tips for employers, training resources, and outreach materials to reduce stress and burnout among workers.
Reduce stigma for service members and veterans. Service members and veterans are at increased risk for mental health challenges. Earlier this month, the Department of Defense (DoD) issued a new policy that makes it easier for Service members to seek support by self-initiating a referral for a mental health evaluation through a commanding officer or supervisor. This policy, based on the Brandon Act, allows Service members to seek confidential help, reducing stigma associated with mental health issues. This month, the Department of Veterans Affairs (VA) is also leveraging its Today I Am Campaign, to showcase veterans’ stories of getting help to inspire other veterans to proactively seek support and resources.
Deliver mental health services to caregivers. To help address the stress of family caregiving, this month, VA launched a pilot program to provide mental health services to caregivers enrolled in the Program of Comprehensive Assistance for Family Caregivers. This new program will address the unique mental health needs of veteran caregivers by providing evidence-based services centered around couples, family therapy, and the individual needs of the caregiver.
Reduce disparities in maternal mental health. Too often, postpartum depression and anxiety go undiagnosed. This month, HRSA will announce awards for more than $65 million to 25 HRSA-funded health centers to implement innovative approaches to improve maternal health outcomes and reduce disparities for women from underserved backgrounds by supporting health centers to partner with patients and the community to develop and pilot innovative, patient-centered, scalable models of care delivery that address the clinical and health-related social needs of health center patients at highest risk of maternal morbidity and mortality. HRSA also just marked the one-year anniversary of the maternal mental health hotline. The 24/7 hotline, 1-833-TLC-MAMA, provides support before, during and after pregnancy and is currently staffed by more than three dozen call-takers, including nurses, doulas, and lactation consultants. During the first year, the hotline received more than 12,000 calls and texts.
Promote behavioral health equity. Earlier this month, SAMHSA launched a Behavioral Health Equity Challenge which will provide up to ten awards to community-based organizations for innovative outreach and engagement strategies that help members of underserved racial and ethnic communities engage in culturally and linguistically responsive services across the continuum of care for behavioral health, including mental health promotion, substance misuse prevention, and treatments and supports that foster recovery.
Create Healthy and Supportive Environments
In addition to investments in the health care system, we must also build environments that promote wellness and recovery and prevent mental health challenges from occurring in the first place. This month, the Biden-Harris Administration is taking new actions to:
Improve youth resilience. Unlike ever before, our kids are facing the consequences of multiple crises at once, from COVID-19 to gun violence among other key issues. HHS announced the new Children and Youth Resilience Prize Challenge, which will award $1 million to innovative community-led solutions to promote resilience in children and adolescents affected by the COVID-19 pandemic and other disasters.
Promote the importance of social connection. Social isolation and loneliness are far too common. People from all walks of life have been forced to grapple with increase social isolation and loneliness, especially due to the COVID-19 pandemic. Earlier this month, the U.S. Surgeon General released a new Advisory on Addressing Loneliness and Promoting Social Connection. And, CDC also launched a new website for adults, which provides key suggestions on how to combat loneliness by improving social connectedness.
Invest in early childhood mental health. Like with physical health, it is important for us to start taking care of the mental health of our children as early in their lives as possible. Later this month, SAMHSA will award $9.7 million in grants through the infant and early childhood mental health program to improve outcomes for children from birth up to 12 years of age via improved interventions and treatment services.
Improve suicide prevention efforts. Beyond scaling up 988, the Administration is also taking additional actions to better prevent suicide. The Indian Health Service (IHS) will implement a system-wide suicide prevention training for all staff to increase recognition and response to suicide within American Indian and Alaska Native populations. Later this month, SAMHSA will award $6 million in suicide prevention grants across multiple programs to support states and tribes with implementing youth suicide prevention and early intervention strategies in schools, institutions of higher education, juvenile justice systems, substance use and mental health programs, foster care systems, and other child and youth-serving organizations.
Launch public call-to-action to support research. This month, the White House Office of Science and Technology Policy called on non-profit organizations, advocacy groups, academic institutions, companies, and other research funders to share their actions and collaborations to help advance national mental health research priorities. This builds on the first-of-its-kind White House Report on Mental Health Research Priorities, which outlined a set of critical and timely needs and opportunities in mental health research.
Improve employee wellness. Americans spend much of their lives working, so it is critical that we foster healthy mental health practices even at work. Later this month, the Administration’s Office of Personnel Management (OPM) will release an Employee Wellness Program Guidance for agencies on best practices for providing wellness services to federal employees. The Administration also launched an interagency Mental Health and Well-being Community of Practice to continue to identify best practices and develop a government-wide toolkit for agencies containing metrics, data, insights, and options for agencies to use to understand and promote employee well-being and mental health.
Expand access to recovery. Treatment works and recovery is possible, and the Administration is committed to supporting all living in recovery. In the coming weeks, SAMHSA will announce $5.4 million in grant awards for building communities of recovery to support mobilization and connection of community-based resources to increase access to and quality of long-term recovery support for people with substance use disorders and co-occurring substance use and mental health disorders.

Artificial Intelligence for Behavioral Health
Artificial intelligence (AI) can transform various aspects of behavioral health diagnosis, treatment, and follow-up monitoring. Here are some new and emerging business opportunities in this field:
AI-Assisted Diagnosis: AI can assist clinicians in diagnosing mental health conditions. Machine learning algorithms can analyze vast amounts of data, such as patient history, symptoms, genetic information, and biomarkers, to provide more accurate and timely diagnoses. Startups can develop AI-powered diagnostic tools or collaborate with healthcare providers to integrate AI algorithms into existing diagnostic processes.
Virtual Mental Health Assistants: AI-powered virtual assistants or chatbots can be designed to provide mental health support and counseling. These virtual assistants can use natural language processing and sentiment analysis to engage in conversations with individuals, offer coping strategies, provide information about available resources, and even monitor changes in mood or behavior over time. Companies can develop and market virtual mental health assistants for clinical and self-help purposes.
Personalized Treatment Plans: AI can help tailor treatment plans to individual patients by analyzing large datasets and identifying patterns in treatment responses. This can enable the development of personalized interventions and recommendations. Startups can leverage AI algorithms to create software tools that assist clinicians in generating personalized treatment plans based on a patient's specific needs and characteristics.
Digital Therapeutics: AI can enhance the effectiveness of digital therapeutics, software-based interventions aimed at preventing, managing, or treating mental health conditions. By leveraging AI algorithms, these digital therapeutics can provide adaptive and personalized interventions, track progress, and adjust treatment plans in real time. Companies can develop and market AI-powered digital therapeutics to improve access and outcomes in behavioral health.
Predictive Analytics for Relapse Prevention: AI can analyze patient data to predict the likelihood of relapse or deterioration in mental health conditions. By identifying early warning signs, clinicians can intervene proactively and prevent crises. Startups can develop predictive analytics models and tools that integrate with electronic health records (EHRs) or remote monitoring systems to provide actionable insights for relapse prevention and treatment adjustments.
Continuous Remote Monitoring: AI-enabled wearable devices and smartphone apps can passively collect behavioral and physiological data, such as sleep patterns, activity levels, heart rate variability, and social interactions. AI algorithms can then analyze this data to provide insights into an individual's mental health status and triggers. Companies can create wearable technologies and AI-driven platforms that enable continuous remote monitoring for behavioral health purposes.
Data Analytics for Population Health Management: AI can analyze large-scale behavioral health datasets to identify population-level trends, risk factors, and patterns. This information can guide public health interventions, resource allocation, and policy decisions. Businesses can develop AI-powered analytics platforms that help healthcare organizations, and policymakers make informed decisions for population health management in the behavioral health domain.
These are just a few examples of the emerging business opportunities in using AI for behavioral health diagnosis, treatment, and follow-up monitoring. The field is rapidly evolving, and entrepreneurs and innovators are exploring new ways to leverage AI to improve mental health outcomes.

Biden plans to combat mental health challenges
Jeanine Santucci (USA Today) America's young people are in a worsening mental health crisis, with factors including isolation during the pandemic school closures, and social media use leading to soaring numbers experiencing depression, anxiety, and suicidal thoughts, research has found. The Biden administration is rolling out plans during Mental Health Awareness Month to address the problem.
The number of teens who experienced persistent feelings of sadness or hopelessness increased in the past decade: 57% of high school girls experienced those feelings in 2021 compared with 36% in 2011, a Centers for Disease Control and Prevention report on youth behavioral health found.
On Thursday's National Day of Mental Health Action, the Biden administration highlighted its efforts to combat mental health challenges, especially among children and teens in school settings. "President Biden knows and believes that mental health is health, period," Susan Rice, President Joe Biden's domestic policy adviser, said on a call with reporters.
Here's a look into what the Biden administration is doing to tackle mental health in the US. :
LONELINESS AFFECTING AMERICANS: A loneliness 'epidemic' is affecting a staggering number of American adults. How the surgeon general plans to fight it.
Mental health in young people
Rice said the nation's mental health problems are even more acute in young people. She cited the CDC report that found 13% of high school girls and 7% of high school boys reported attempting suicide in the past year when surveyed in 2021. More than one-fifth of all high school students said they seriously considered it.
Schools to receive influx of funding to hire more therapists
The White House highlighted the recent announcement that 35 states would receive more than $95 million in funding from the bipartisan Safer Communities Act to improve school-based mental health services. The funding is estimated to add 14,000 mental health professionals such as counselors, psychologists and social workers.
The money will add about 2,631 new mental health professionals to schools in Illinois, 400 in Massachusetts, five in Utah and 36 in Delaware, for example.
The administration said it is also working to make it easier for schools to bill Medicaid for mental health services under new guidance from the Department of Health and Human Services.
Biden's commitment on mental health
During his first State of the Union address, Biden announced mental health was one of the key pillars of his Unity Agenda, which sought to bring members of the Republican and Democratic parties together to tackle issues that also included cancer research, caring for veterans and dealing with the opioid epidemic.
The White House said Thursday that Biden's objectives going forward to address mental health for children and adults include "strengthening the mental health workforce and system capacity, connecting more Americans to care, and creating a continuum of support."
Rice said the Department of Health and Human Services will provide $200 million more in funding to scale up operations for 988, the mental health crisis hotline launched last year.ke a minute to write an introduction that is short, sweet, and to the point.
Arizona Behavioral Health: Turning Crisis into Transformation
Policy Priorities 2023
Arizona is facing a mental health and substance abuse crisis never seen before. A problem exacerbated by the ongoing pandemic, the availability of opioids such as fentanyl, and healthcare workforce shortages resulting in a dramatic increase in the need for care and diminished access to it.
This behavioral health crisis is impacting Arizona's economic vitality and competitiveness. Sound physical and mental health are essential ingredients for a productive workforce.
However, individuals with mental illness and substance use disorders are less likely to acquire and maintain the skills for successfully participating in the labor force. This creates high costs for employers to recruit, train and retain skilled workers. Serious mental illness costs the U.S. economy more than $318 billion annually through absenteeism, unengaged workers, disability, healthcare costs, and lost productivity.
During the past year, the Health Communities and Wellness Alliance has surveyed education, industry, nonprofit, and public sector leaders in Southern Arizona on high-priority action steps to pursue. Three areas are highlighted as critical priorities.
Accelerate the Talent Pipeline
The top priority is to address the behavioral health workforce shortage in Southern Arizona so that access to services is widely available.
Social Determinants of Health
A second priority is addressing Social Determinants of Health (SDOH) that interact and compound to create significant behavioral health disparities in low-income areas. People living in poverty have limited access to employment, healthy food, safe housing, transportation, and quality healthcare. Addressing these underlying factors is essential for improving health in these communities.
Disruptive Innovation.
A third priority. The moment is ripe for disruptive innovation and leveraging emerging technologies to address this challenge across multiple fronts. The opportunities include leveraging new digital technologies, holistic treatment strategies, biome diagnostics, telehealth, in-home monitoring, collaborative care, on-demand virtual training, data analytics, artificial intelligence, and immersive environments for personal lifestyle skills. Wellness depends on integrating health's physical, mental, emotional, and spiritual dimensions.
SAMHSA Seeks Billions to Bolster Mental Health and Substance Use Services Across the Nation
March 13, 2023. The President’s Budget for Fiscal Year (FY) 2024 includes $10.8 billion for the Substance Abuse and Mental Health Services Administration (SAMHSA), $3.3 billion over the agency’s FY 2023 enacted budget. The FY 2024 budget proposal continues to support the President’s Unity Agenda to address the national mental health crisis and overdose epidemic.
With a multidimensional approach to addressing the nation’s behavioral health challenges, SAMHSA’s FY 2024 budget proposal includes a historic investment to transform America’s behavioral health crisis care system, with the expansion of the 988 Suicide & Crisis Lifeline; a mandatory proposal for Community Mental Health Centers (CMHCs) to increase access to high-quality, comprehensive mental health services in communities across the nation; and the request to Congress to change ‘Abuse’ to ‘Use’ in the Agency’s and Centers’ names, to reduce the historic stigma that too often has proven to be a barrier to seeking and receiving care.
“The Fiscal Year 2024 SAMHSA budget proposal contains critical, targeted investments to address America’s behavioral health needs and to increase access to quality care for individuals and families across the nation,” said Miriam E. Delphin-Rittmon, Ph.D., the Health and Human Services’ Assistant Secretary for Mental Health and Substance Use and the leader of SAMHSA. “This funding will further facilitate SAMHSA’s daily work to connect more people to proven prevention, treatment, and recovery services and supports.”
Targeted investments to improve the mental health and well-being of individuals and families across the country include:
$1.7 billion, an increase of $645 million, for the Community Mental Health Services Block Grant. The two-year funding to states includes a 10 percent set-aside for evidence-based programs for individuals with early serious mental illness (SMI), including first-episode psychosis; a proposal to increase the crisis care set-aside from 5 to 10 percent; and a new 10 percent set-aside for evidence-based programs to support at-risk youth and adults.
$413 million for Community Mental Health Centers (CMHCs) operated by state and local governments, as well as nonprofit organizations, to increase access to high-quality, comprehensive mental health services in communities across the nation. The budget proposal will further expand the range, quality, and capacity of services in CMHCs, building on the $825 million in funding directed to CMHCs in the Coronavirus Response and Relief Supplemental Appropriations.
$553 million, an increase of $168 million, for Certified Community Behavioral Health Clinics (CCBHCs). The funding would further increase access to and coordination of care to enable individuals to receive timely diagnosis, treatment, and recovery support services. The budget proposal also includes a request for authority to develop a process for accrediting CCBHCs.
$836 million, an increase of $334 million, to the 988 Suicide & Crisis Lifeline. From July to December 2022, the 988 Lifeline answered more than 2.1 million contacts. The requested funds, to be dispersed to states, local crisis centers, tribes and tribal organizations, and the system administrator, would scale and strengthen the 988 crisis care operation to respond to the 9 million contacts anticipated in FY 2024.
$244 million, an increase of $104 million, for Project Advancing Wellness and Resiliency in Education (AWARE), which identifies children and youth in need of mental health services in their schools. Since the COVID-19 pandemic began, anxiety, depression, loneliness, and negative emotions and behaviors have increased among young people—with many saying they have considered or attempted suicide. In FY 2024, SAMHSA projects these funds will help to identify and refer approximately 120,000 school-aged youth to mental health and related services.
$102.9 million, an increase of $47 million, for Primary and Behavioral Health Care Integration, which expands the infrastructure and increases the availability of primary health care and wellness services for individuals with SMI or co-occurring mental illness and drug/alcohol addiction. This is particularly crucial because many Americans see their primary care physicians about behavioral health needs before seeing behavioral health care providers. In FY 2022, this effort trained 62,806 individuals in the mental health and related workforce.
Investments focused on keeping people who use drugs alive and increasing access to prevention, treatment, and recovery services and supports for individuals with substance use disorders include:
$2 billion, an increase of $425 million, for the State Opioid Response (SOR) grant program, which disperses funding to states and territories to address the public health crisis caused by escalating opioid misuse and substance use disorder across the nation. Of the $2 billion, $75 million would go to the corresponding Tribal Opioid Response (TOR) grant program. Since the SOR program began, approximately 1.2 million patients have received treatment services, including more than a half-million who have received an FDA-approved medication for opioid use disorder. The budget increase would enhance states’ ability to address stimulants (such as methamphetamine and cocaine), as well as other issues related to the overdose epidemic.
$2.7 billion, an increase of $700 million, for the Substance Use Prevention, Treatment and Recovery Support Block Grant. With an updated name that sheds stigmatizing language, the block grant works to ensure that individuals, their families, and communities across the country have access to substance use-related prevention, treatment, harm reduction, and recovery support services necessary to improve individual outcomes and reduce the impact of substance misuse. The budget proposal includes a request for a 10 percent set-aside for recovery support services to significantly expand the continuum of care. FY 2022 block grant funding has connected more than 205,000 people to withdrawal management services; more than 329,000 people to residential treatment levels of care; 883,000 people to ambulatory services; and 343,000 people to outpatient treatment that included medications for opioid use disorder.
$50 million to Community Harm Reduction and Engagement Initiatives, a new program that would fund state, local and territory governments, as well as tribal and nongovernmental efforts to address the gap in substance use care by supporting broad-based community harm reduction activities and linkages to services. The program would reach approximately 330,000 people with harm reduction and low-threshold treatment services through resources for community-based organizations, community harm reduction and engagement expansion grants, and a technical assistance center.
The budget also seeks to update SAMHSA’s and its centers’ names to remove the stigmatizing label of “substance abuse,” a change that requires Congressional action. View the SAMHSA budget proposal (PDF | 8.6 MB).int.
IMPACT REPORT
Reviewing the Alliance start-up year and major priorities for 2023.
2022 MILESTONES
Established the Alliance as a nonprofit corporation in Arizona toward IRS designation as a 501 c 3 tax-exempt entity.
Mapped the Southern Arizona ecosystem of organizations involved with behavioral health.
Published the Alliance website providing the mission, vision, innovation model, focus areas, grant opportunities, benefits, and donation options.
Identified regional job vacancies in behavioral health occupations and quantified the workforce supply gap.
Completed survey and zoom meetings with thirty leading stakeholders to assess regional behavioral health challenges.
Participated in conferences and workshops to shape regional and federal healthcare policies.
·Supported partner grant initiatives to boost the behavioral health talent pipeline, community flourishing strategies for low-income neighborhoods, and on-demand point-to-point mobility as a social determinant of health.
·Released "Grant Alert" reports highlighting current and forecasted funding opportunities.
Hosted first in-person event with workforce stakeholders to advise on Alliance strategies for 2023.
Federal Funding Bill Provides $10B Toward Behavioral Health in 2023
The Omnibus funding bill includes over $10 billion for behavioral health initiatives. These include $4.9 billion in funding to address opioid abuse and $5.27 billion for mental health treatment, prevention, and research initiatives. Mental health funding is up about 18%, while funding to address opioid abuse is up about 6%, according to summaries provided by Democrats and Republicans from the Senate Appropriations Committee. Overall, these two segments saw a 12% funding increase.
Behavioral health workforce funding is up
Behavioral health workforce development efforts total at least $197 million for fiscal 2023. These include the Behavioral Health Workforce Education and Training program and Mental and Behavioral Health graduate education programs. Funding for these behavioral health-specific programs is up 22% compared to fiscal 2022.
While not explicitly dedicated to behavioral health, funding for the National Health Service Corps is up 33% to $125.6 million. The National Health Service Corps offers loan forgiveness and scholarships in exchange for professionals working in specific medical fields in areas with provider shortages. The Health Resources and Services Administration oversees it.
For fiscal 2022, 41%, or about 10,000, of the roughly 24,600 professionals in the National Health Service Corps worked in the mental health field, according to HRSA data.
Telehealth extensions
The legislation includes provisions to extend and expand telehealth flexibilities through Dec. 31, 2024. Under current law, many of these flexibilities were set to expire 151 days after the end of the COVID-19 PHE. These include:
· Expanding originating site to include any site at which the patient is located, including the patient’s home.
· Expanding eligible practitioners to furnish telehealth services to include occupational therapists, physical therapists, speech-language pathologists, and audiologists.
· Extending the ability for federally qualified health centers (FQHCs) and rural health clinics (RHCs) to furnish telehealth services.
· Delaying the six-month in-person requirement for mental health services furnished through telehealth, including the in-person requirements for FQHCs and RHCs.
· Extending coverage and payment for audio-only telehealth services; and
· Extending the ability to use telehealth services to meet the face-to-face recertification requirement for hospice
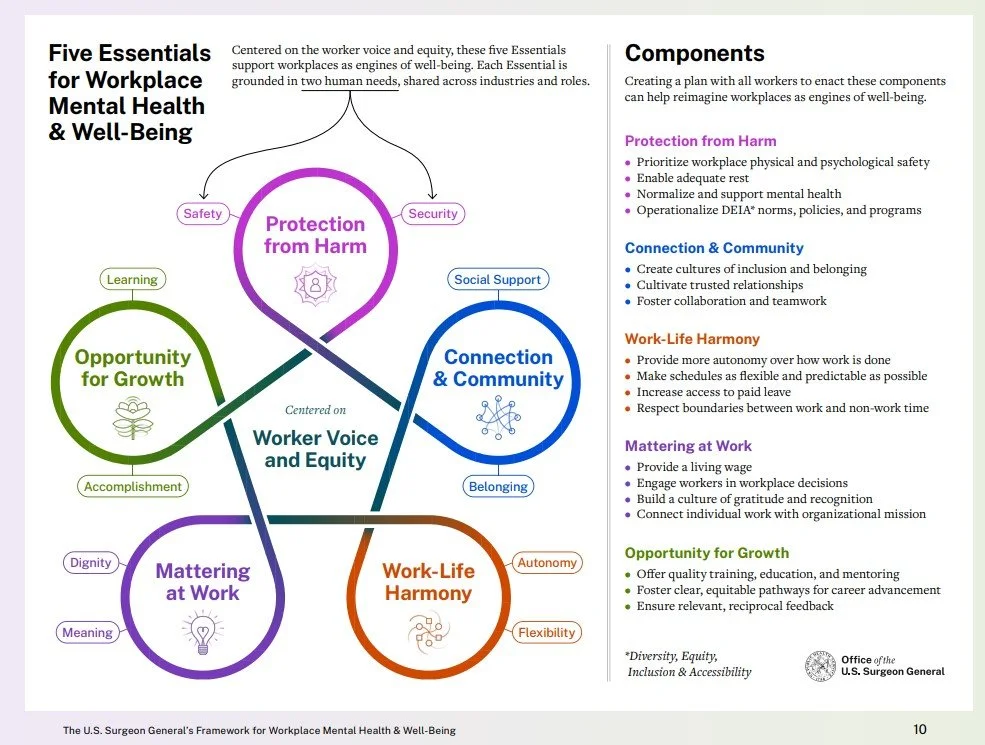
Workplaces Can Be Engines of Mental Health and Well-Being
We can build workplaces that are engines of well-being, showing workers that they matter, that their work matters, and that they have the workplace resources and support necessary to flourish.
This 30-page Surgeon General’s Framework for Workplace Mental Health and Well-Being offers a foundation that workplaces can build upon. Download the document PDF.
Funding opportunity to demonstrate innovative transportation service to improve behavioral health.
A new USDOT competitive funding program offers $2 million phase one grants to municipal-led partnerships to organize, plan, and design high-tech prototype mobility systems in an 18- month project effort. No dollar match is required. Implementation will be funded in phase two efforts competitively funded by USDOT for up to $15 million over three years. Officially designated "transportation disadvantaged communities" are a target for phase one funding. Multiple government entities are eligible (i.e., Tucson City, Pima County, tribes, and transit agencies).
Project Prospectus prepared by Alliance and CATES. DOWNLOAD
Envisioned Mobility System
Access to affordable, on-demand, point-to-point transportation is a significant Social Determinant of Health (SCOH). A new mobility mode of automated, remotely monitored passenger vehicles is emerging to supplement existing modes with no traveler requirement to use a car or wait at a bus stop. Safe, affordable, environmentally friendly, electric-powered passenger mobility on urban streets for all residents and visitors is becoming more workable every month. There is a clear path to setting up motorized, financially sustainable, equitable, on-demand universal mobility in the Greater Tucson Region, including access to transit stations, healthcare facilities, childcare services, education institutions, food stores, workplaces, churches, etc. Especially valuable to residents and visitors who do not have access to personal vehicles.
Tucson and Pima County are in excellent positions to compete for SMART funding because of designated "transportation disadvantaged communities" and the capability to understand and embrace the potential of electric and automated vehicles' passenger mobility.

Improving mental health on World Mental Health Day
There’s no shortage of external triggers that have affected our mental health and well-being: the COVID-19 pandemic, subsequent widespread employee burnout, and other global and regional crises like climate change. It’s a tough time for Gen Z, who are reporting poorer mental health compared with older generations, write Erica Hutchins Coe, Martin Dewhurst, and coauthors in a recent McKinsey Health Institute survey. On #WorldMentalHealthDay, dive deeper with these insights about the state of mental health around the world and what organizations can do to address pressing issues related to mental health.
Leading with compassion: Prioritizing workplace mental health
Toxic workplace behavior and employee burnout: Fix one, fix both
Heat waves, the war in Ukraine, and stigma: Gen Z’s perspectives on mental health
Beyond burnout: What helps—and what doesn’t
In sickness and in health: How health is perceived around the world
Addressing employee burnout: Are you solving the right problem?
‘Be brave, not perfect,’ says mental health advocate Poppy Jaman
‘When it comes to mental health, all countries are developing countries’
Employee mental health and burnout in Asia: A time to act
Author Talks: We need to talk about Asian American mental health
World Mental Health Day, is an international day for global mental health education, awareness, and advocacy against social stigma. It was first celebrated in 1992 at the initiative of the World Federation for Mental Health, a global mental health organization with members and contacts in more than 150 countries. Wikipedia
Observed by: World Federation for Mental Health, World Health Organization, and member organizations of WFMH
Arizona tribes are eligible for grants for the 988 crisis line
The U.S. Department of Health and Human Services is making $35 million available in grants to Native Americans to help implement a nationwide mental health crisis hotline. Arizona has more than 20 federally recognized tribes.
The 988 hotline went live in July. It's an easy number to remember, similar to 911. The hotline connects callers with trained mental health counselors. The money available to 574 federally recognized tribes will have a limited reach, with up to 100 grants awarded. The deadline to apply is Oct. 25.
Native Americans and Alaska Natives are disproportionately impacted by suicide, according to Federal data.
These grants ( cooperative agreements) provide resources to improve response to 988 contacts (including calls, chats, and texts) originating in Tribal communities and activated by American Indians/Alaska Natives. This program aims to: (1) ensure American Indians/Alaska Natives have access to culturally competent, trained 988 crisis center support; (2) improve integration and support of 988 crisis centers, Tribal nations, and Tribal organizations to ensure there is navigation and follow-up care; and (3) facilitate collaborations with Tribal, state, and territory health providers, Urban Indian Organizations, law enforcement, and other first responders in a manner which respects Tribal sovereignty.
LINK: https://www.samhsa.gov/grants/grant-announcements/sm-22-020

Why it is awesome that your brain can experience awe
Experiencing awe is associated with lower stress and inflammation levels, and a higher sense of meaning and connection, research shows
By Richard Sima, Washington Post
September 15, 2022
Not many people have held a human brain in their hands, but I am among a lucky few.
I remember the weight of it, both physical and metaphorical. The brain itself was probably three pounds of flesh — firm but pliable to the touch, and smelling strongly of preservative. I cupped it in both hands for fear of dropping it.
Holding the brain, I couldn’t help but think how this was a person in my hands, and their thoughts, feelings, hopes, fears and dreams — a whole life — were embodied in its folds and creases.
At the time, I could not name exactly what I was feeling — the giddiness, the slight lightheadedness, the catching of the breath — but looking back, I know I was feeling awe.
The benefits of seeking awe
As a neuroscientist-turned-science-journalist, one of my goals in writing this weekly column is to reveal the wonder and mystery of the brain, and why it matters in our everyday lives. And there’s no better place to start than to explore our ability to experience awe, and how seeking awe-inspiring experiences can improve our well-being.
Awe has two fundamental components, say researchers who study the emotion. It is a response to encountering something more vast, complex, or mind-blowing than we had conceived of either physically or conceptually. The experience also induces a change in how we see the world, producing “little earthquakes in the mind.”
To understand the concept of awe, it helps to know how the brain responds to what we perceive as mundane. Over the course of our lives, our brains learn and encode what “normal” is and predict what we think should happen next, based on our internal understanding of the world.
“That prediction of what happens next guides our behavior. It is crucial for being able to function in this incredibly complicated world,” said Michelle “Lani” Shiota, an associate professor of social psychology at Arizona State University. “But it does narrow our perspective, it narrows our vision. And it simply doesn’t account for everything.”
Awe might be our most undervalued emotion. Here’s how to help children find it.
Research has repeatedly found that experiencing something extraordinary may make us (and our worries) feel small. And not in a bad way.
“You know, by adulthood, we move through the world pretty immersed in our own concerns, our own minutiae of the day-to-day, our own responsibilities, and it can be hard to keep a sense of perspective about how that fits into the grand scheme of things,” Shiota said.
Experiencing more awe is associated with living healthier and more meaningful lives. A 2021 study reported that feeling more awe is correlated with reporting feeling lowered levels of daily stress. Intriguingly, people who feel more awe also tend to have lower levels of inflammatory cytokines. Positive experiences of awe have also been found to increase feelings of well-being, life satisfaction and sense of meaning.
By becoming less attuned to ourselves and more attuned to the rest of the world, awe helps us re-contextualize ourselves, said Paul Piff, an associate professor of psychological science at the University of California at Irvine. “It helps make you feel like there’s more going on in the world than just you. And it gives you that sense of being a part of something much bigger than yourself,” he said.
Emerging research shows that experiencing awe may make us more curious, creative and compassionate people. And in turn, recent studies have found, awe-prone people may be more prone to being curious, and people who experience more awe also tend to be more creative.
How gazing into the Grand Canyon and other awe-inspiring moments can make you a more generous person
Awe leads people to feel more connected with others and identify with more universal categories such as “a person” or “inhabitant of earth,” as opposed to more individualistic, limited ones.
In different studies, when researchers induced awe in participants in laboratories, such as by showing panoramic clips of places on Earth, people behaved more prosocially, being more likely to help out, donate more money and volunteer more time for strangers.
By transforming our sense of self and meaning, and enhancing our relationship with others and the wider world, awe has the power to improve our mental and physical health.
Eliciting awe in the every day
You don’t need to visit the Grand Canyon, witness the birth of your child or hold a brain to experience awe. The awe-inspiring is all around you.
“Awe is related to this sense of oneness with humankind,” Piff said. “I think you can have your mind blown in more mundane, minuscule ways in even everyday settings.”
While more research needs to be done on what best elicits awe, many paths lead to awe.
Piff offers these suggestions:
· Viewing something giant such as a mountain range or ocean.
· Discovering something tiny such as the worlds seen through a microscope.
· Contemplating a piece of music or (re)discovering a piece of art.
· Taking “awe walks” through your neighborhood or in nature, which is a never-ending source of awe.
His favorite suggestion, though, is to just take a walk out the door. Once you step outside, pick a random number between 1 and 100. Take that number of steps, and look beneath your feet. If you look around to find something inspiring, odds are you will, Piff said. “And I bet you, when you’ve tried to do it, you will do it,” he said.
Nature can affect human well-being in many more ways than you think
The awe-inspiring is also within you.
Not everyone will have the experience of holding a brain in their hands, but we are blessed with a brain conveniently held in our head.
Our brains are capable of astounding mental achievements — launching spaceships to planets millions of miles away, creating effective vaccines to combat pandemics — and coordinating our bodies to perform physical feats.
But your brain is performing equally wondrous functions right this instance, perhaps without you knowing.
Your brain is perceiving squiggles on a page and transforming them into meaning, while putting them into a broader context by remembering what came before. It is filtering out extraneous sounds around you, the touch of clothing on your skin. Because of your brain, you are simultaneously maintaining the muscle tone to keep whatever posture you are in and breathing unconsciously (though perhaps now no longer).
Your brain — 80 billion-some neurons relaying electrical and chemical signals across approximately 100 trillion connections — is sensing, feeling, deciding, evaluating, planning, adjusting and keeping you alive.
And in considering all these concurrent acts and duties, you are maybe even experiencing a twinge of awe, a feeling our brain allows us to experience — and is also a source of.
And that is pretty awesome.
Healthy Pima
The 2021 Community Health Needs Assessment (CHNA) has been released. This report is the result of community collaboration and identifies health priorities for Pima County and proposed solutions to health challenges.
Top health priorities include:
Mental and Behavioral Health
Social Determinants of Health
Access to Care
Substance Use Disorder







